What is peripheral artery disease?
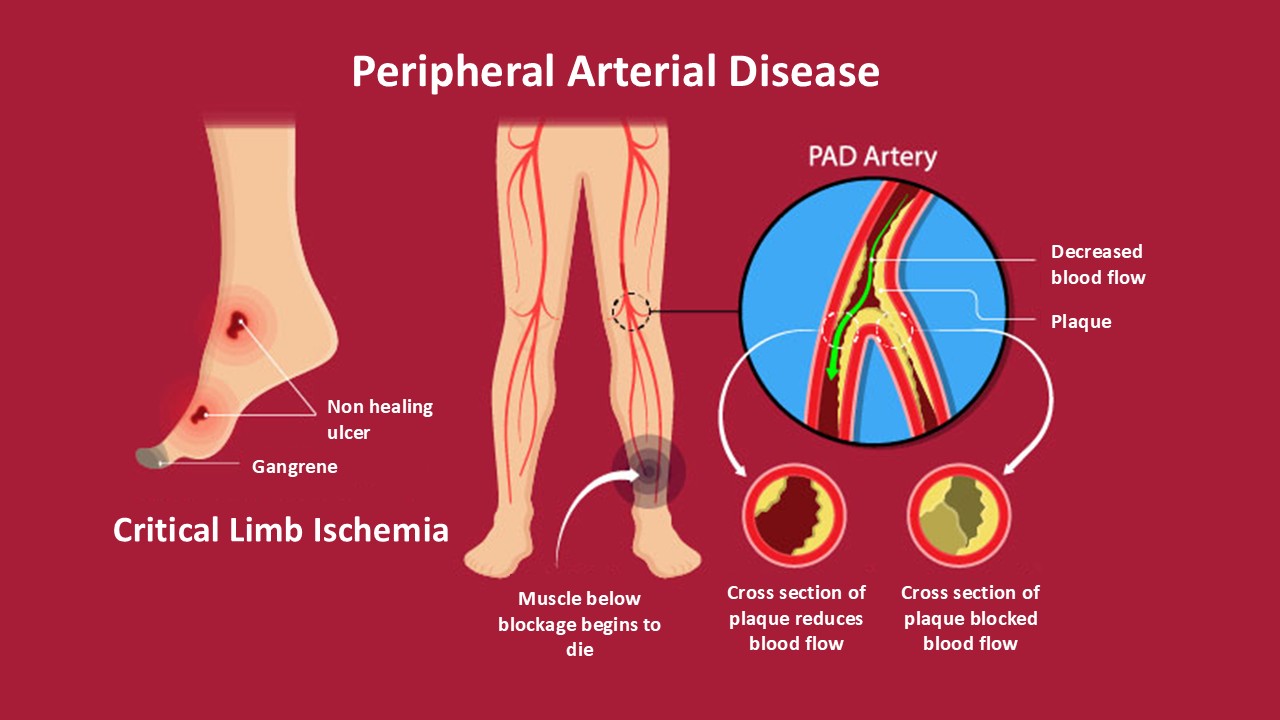
Peripheral artery disease (PAD) is often caused by a buildup of fats, cholesterol and other substances in and on the artery walls, a condition called atherosclerosis. The buildup is called plaque. Plaque can cause arteries to narrow, blocking blood flow.
Due to malfunctions or blockages in your arteries, your body’s ability to pump oxygenated blood to your legs or other limbs can cause severe leg pain, leg cramps when walking, difficulty healing wounds on the feet or lower leg and an eventual need for amputation.
PAD primarily affects the legs but can also damage arteries in the kidneys, abdomen, feet, ankles, pelvis, hips, buttocks and arms. PAD is most common in adults over age 50, and is often associated with diabetes, high cholesterol and high blood pressure – but it can also occur in younger people. People who smoke or are obese are at a higher risk of developing PAD early in life.
Peripheral artery disease (PAD) affects 1 in 20 of America’s adult population over age 50, and more than half of limb amputation patients lost their limbs due to PAD and other vascular diseases.
Peripheral artery disease (PAD) is a common condition. It’s often treated with medicines and a walking program. But severe PAD can lead to complications, including gangrene and potential amputation.
What is limb salvage?
Limb salvage is a multidisciplinary program designed to identify diseased limbs (legs and feet) and repair and/or restore blood supply, tissues or muscles with the goal to preserve the mobility and functionality of the limb and minimize amputation.
What are the risks and causes associated with limb salvage?
• A family history of peripheral artery disease, heart disease or stroke
• Diabetes
• High blood pressure.
• High cholesterol
• Increasing age, especially after 65, or after 50 if you have risk factors for atherosclerosis
• Obesity
• Smoking
Suffering any one of these conditions can mean that you have severely limited blood flow to your lower limbs, and ignoring these conditions can lead to serious complications. Finding the right limb salvage team is important when treating your leg/feet disease before the damage is too extensive to repair.
Peripheral artery disease (PAD) may not cause symptoms, or symptoms may be mild. PAD symptoms include:
- Pain when walking
- Foot pain at rest (rest pain)
- Sores on your legs and feet that are slow to heal
- Leg cramps during exercise (claudication)
- Numbness of the feet
- Temperature changes in the feet/legs
- Leg or foot coloration changes
- Slower growth in toenails
How is PAD diagnosed?
- Ankle-brachial index (ABI). This is a common test used to diagnose PAD. It compares the blood pressure in the ankle with the blood pressure in the arm. You may be asked to walk on a treadmill. Blood pressure readings may be taken before and right after exercising to check the arteries during walking.
- Ultrasound of the legs. Sound waves create pictures of how blood moves through the blood vessels of the legs or feet. Doppler ultrasound is a special type of ultrasound used to spot blocked or narrowed arteries.
- Angiography. This test uses imaging tests and a dye to look for blockages in the arteries. The dye is given through a blood vessel. It helps the arteries show up more clearly on the test images.
How is PAD treated and prevented?
Smoking cessation
Tobacco smoke is a major risk factor for PAD and increases your risk for heart attack and stroke. If you smoke, take steps to quit. Effective tools include behavior modification programs, nicotine replacement medicines and other quit-smoking medications. Quitting smoking will help slow the progression of PAD and other heart-related diseases. Ask your health care professional for guidance to help you quit.
Physical activity
An effective treatment for PAD symptoms is regular physical activity. Your health care professional may recommend supervised exercise training, also known as supervised exercise therapy, or SET. You may have to begin slowly, but simple walking regimens, leg exercises and treadmill exercise programs can ease symptoms.
Exercise for leg pain (intermittent claudication) considers that walking causes pain. The program consists of alternating activity and rest in intervals to build up the amount of time you can walk before the pain sets in. It’s best if this exercise program is done in a rehabilitation center on a treadmill and monitored. If it isn’t possible to go to a rehab center, your health care professional may recommend a structured community or home-based program.
Diet
Many people with PAD have elevated cholesterol levels. A diet low in saturated and trans-fat can help lower blood cholesterol levels. Cholesterol-lowering medication may also be needed.
Aim for a healthy diet that emphasizes vegetables, fruits and whole grains. Include low-fat dairy products, poultry, fish, legumes, nuts, seeds and non-tropical vegetable oils such as olive oil. Choose foods that are unprocessed or minimally processed. Limit sodium, saturated and trans fats, added sugars, sugar-sweetened beverages and red meat.
Medication
It’s important to take the medication that your health care professional prescribes. Not taking these medications can increase your risk for PAD, as well as heart attack and stroke. Medications that may be prescribed include:
Antiplatelet medication, such as aspirin and/or clopidogrel, to prevent blood clotsCholesterol-lowering medications, such as statins
High blood pressure medications (In people with PAD and high blood pressure, angiotensin-converting enzyme inhibitors or angiotensin-receptor blockers are recommended.)
Oral anti-coagulants, such as rivaroxaban, to decrease the tendency for blood clots to form
If you have claudication, you also may be prescribed medication (cilostazol) to help improve your walking distance and decrease leg symptoms.
Managing diabetes
Diabetes increases the risk of poor outcomes among people with PAD. Achieving glucose control benefits all people with diabetes and can reduce limb-related complications in those with PAD.
Work with your health care team to create a coordinated care plan, including:
- A healthy diet to reduce your cholesterol and manage diabetes
- Reaching and maintaining a healthy weight
- Medications for glucose management
- Managing other cardiovascular risk factors
- Foot care and ulcer prevention
Procedures
- Aortagram is a specialized X-ray, or angiogram, that uses contrast dye and a catheter to visualize the aorta, identifying blockages, aneurysms, dissections, or narrowing in the aorta and its branches. It is used to diagnose vascular conditions or guide, with the procedure typically involving catheter insertion in the groin.
- Procedure steps: A catheter is inserted, usually via the femoral artery in the groin, and guided to the aorta.
- Contrast Dye: Contrast dye is injected through the catheter, allowing X-ray imaging of blood flow.
- Imaging: X-ray pictures (often digital subtraction angiography) are taken to map the vessel structure.
- Duration: The procedure typically takes about an hour.
- Access point: Usually by inserting a catheter through an artery in the wrist (radial) or groin (femoral)
- Angioplasty is a minimally invasive, procedure used to open blocked arteries by inflating a small balloon at the site of blockage, often placing a stent to keep it open. It is highly successful in restoring blood flow and relieving chest pain, with recovery typically within a few days, though it requires avoiding heavy lifting for a week or more.
- Procedure Steps: A guide wire is inserted, followed by the balloon catheter, which is inflated to widen the artery. A stent is often deployed during this time to maintain the artery’s openness.Imaging: X-ray and contrast dye (angiography) are used to visualize the blockage and guide the catheter.Duration: The procedure typically lasts 30 to 90 minutes.Anesthesia & Comfort: Conscious sedation (moderate sedation) uses medications to induce a relaxed, sleepy state while allowing the patient to remain conscious, breathe independently, and respond to stimulation.
- Leg bypass surgery is a vascular procedure that creates a new pathway for blood flow around a blocked artery in the leg using a graft (a vein from your body or a synthetic tube). Surgeons make incisions in the leg, clamp the blocked artery, and stitch the graft above and below the blockage to restore circulation, typically taking 1 to 5 hours.
- Types of Bypass: Common types include femoral-popliteal (fem-pop) (groin to knee/below knee) and femoral-tibial (groin to lower leg/ankle).
- Graft Selection: Surgeons prefer using the patient’s own saphenous vein, but synthetic materials like PTFE or Dacron are used if the vein is unavailable.
- Anesthesia: General or spinal anesthesia is administered.
- Access: A 4-to-8-inch incision is made in the thigh or groin area.
- Bypass: The graft is sewn to the artery above the blockage, tunneled under the skin, and attached below the blockage.
- Closure: Incisions are closed with staples or stitches.
- Recovery: Patients usually spend 3 days in the hospital, with a full recovery taking 6 to 8 weeks.
Contact Us
Health care professionals:
Call our dedicated referral line to begin a seamless and streamlined patient referral process.
Referral line: (405) 608-3800
Fax: (405) 972-7542
Email: [email protected]
Oklahoma Heart Hospital North
Limb Preservation Clinic
4050 West Memorial Road
Oklahoma City, OK 73162
Patients with questions should contact Oklahoma Heart Hospital at (405) 608-3800.
Meet Our Team
Mazen Abu-Fadel, M.D., F.A.C.C, F.S.C.A.I.
Beau Hawkins, M.D.
Thomas A. Hennebry, M.D., F.A.C.C.
Benjamin Harkess, D.P.M.
Lenny D. Stubbs, M.D.
Jeffrey Rhodes, M.D.
Ronald R. Magee, M.D.
J. Frank Oaks, D.O.
